The Cornea and Its Importance in Sight
The cornea is a transparent, dome-shaped structure at the front of the eye that acts like a window, focusing light onto the retina. Its clarity and shape are crucial for sharp, accurate vision. The cornea has multiple layers, including the epithelium, stroma, and endothelium, each serving a vital purpose. The epithelium protects against dust, bacteria, and minor injuries, while the stroma provides structural strength. The endothelium maintains fluid balance to keep the cornea clear. Damage from infection, trauma, or degenerative conditions can compromise its function. Understanding how the cornea works emphasizes why corneal transplants are sometimes necessary to restore vision.
What Is a Corneal Transplant?
A corneal transplant, also called keratoplasty, is a surgical procedure that replaces a damaged or diseased cornea with healthy donor tissue. This surgery can be full-thickness or partial, depending on the patient’s condition. The main types of corneal transplant include:
- Penetrating keratoplasty: full-thickness replacement
- Lamellar keratoplasty: selective layer replacement
- Endothelial keratoplasty: innermost layer replacement
The surgeon carefully aligns the donor tissue to maximize clarity and minimize complications. The procedure is typically performed under local or general anesthesia and lasts one to two hours. Postoperative care is essential to ensure the transplant heals properly. Patients usually return home the same day or after a short hospital stay.
Conditions That Require Corneal Transplant
Certain eye conditions make corneal transplantation necessary. These include:
- Scarring from infections or injuries
- Keratoconus, which causes the cornea to thin and bulge
- Inherited corneal dystrophies
- Complications from previous eye surgeries
- Trauma or chemical damage to the eye
Patients with these conditions often experience significantly impaired vision. Corneal transplant offers a solution to restore clarity and improve quality of life. Proper evaluation ensures that the surgery is appropriate for the patient’s needs.
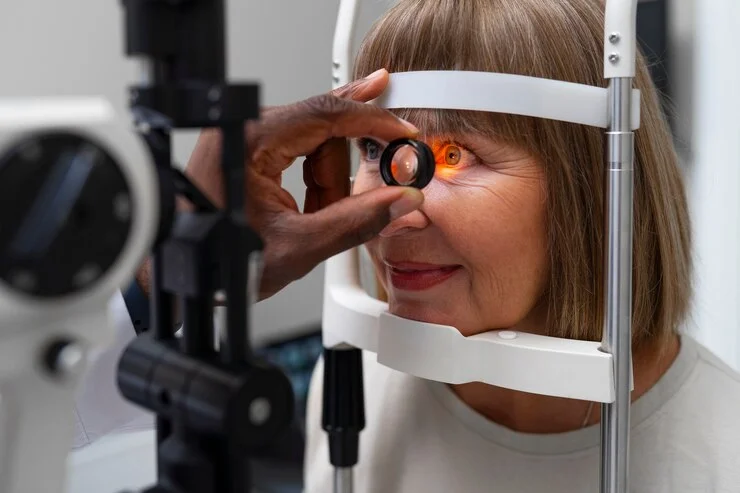
Preparing for Surgery
Preparation is a key part of corneal transplant success. Doctors conduct detailed examinations to evaluate eye health and determine the right surgical approach. Imaging tests measure corneal thickness, shape, and overall condition. Selecting a compatible donor cornea is critical for reducing the risk of rejection. Patients are guided on what to expect, including activity restrictions and medications. Emotional preparation helps patients remain calm and confident during recovery. Clear communication with the ophthalmologist ensures realistic expectations and peace of mind.
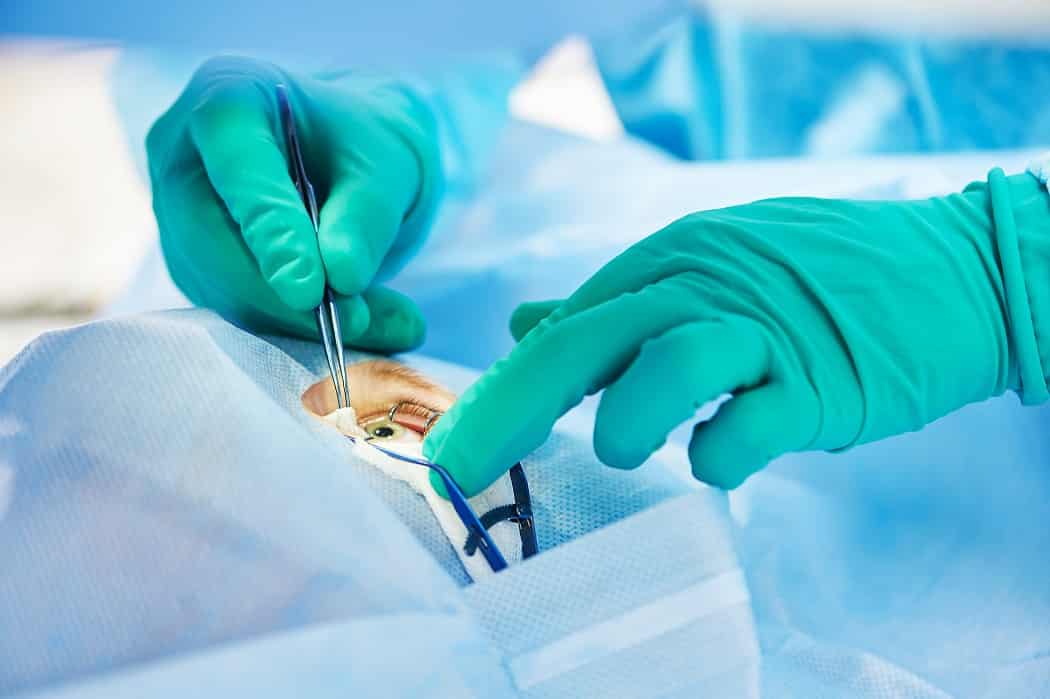
The Surgical Procedure
The procedure begins with anesthesia to prevent discomfort. The damaged portion of the cornea is removed, and donor tissue is precisely placed. Sutures may be used to hold the new tissue in position. Advanced microscopes and surgical tools provide high precision and safety. The surgery usually takes one to two hours. Afterward, the eye is closely monitored for pressure and proper cornea placement. Protective eyewear and postoperative instructions help safeguard the new tissue during initial healing.
Recovery and Postoperative Care
Healing from a corneal transplant is gradual and requires patience. Patients may experience blurred vision, mild discomfort, or swelling in the first few weeks. Eye drops, including antibiotics and anti-inflammatory medications, are prescribed to prevent infection and reduce inflammation. Regular follow-ups allow doctors to track healing and detect complications early. Strenuous activities should be avoided, and protective eyewear is recommended. Vision typically improves over several weeks to months, with full recovery taking up to a year. Following medical guidance is essential for optimal results.
Risks and Complications
Corneal transplant carries some risks, as with any surgical procedure. Graft rejection occurs when the immune system attacks the donor tissue and can manifest as redness, pain, light sensitivity, or blurred vision. Other potential complications include infection, suture-related issues, and increased intraocular pressure. Long-term risks may involve recurrence of the original corneal condition or gradual thinning of the transplant. Consistent use of medications and routine eye exams help reduce risks. Early recognition and treatment of problems significantly improve outcomes. Being informed helps patients take proactive steps during recovery.
Vision Improvement After Surgery
Most patients notice gradual improvement in vision within weeks, while complete stabilization can take months. Success depends on factors such as overall eye health, age, and type of transplant. Some patients may require glasses or contact lenses to achieve optimal vision. Regular eye assessments ensure the cornea remains clear and healthy. Visual improvements enhance daily activities and overall quality of life. Patients who follow postoperative instructions carefully often experience the best outcomes. Understanding the recovery process helps patients maintain realistic expectations.
Advances in Corneal Transplantation
Modern medical advances have significantly improved corneal transplant outcomes. Endothelial keratoplasty allows selective layer replacement, leading to faster healing and reduced risks. Stem cell therapy and regenerative medicine are emerging as promising ways to repair damaged corneas without full transplants. Artificial or bioengineered corneas provide options when donor tissue is unavailable. Advanced surgical instruments and imaging improve precision during the procedure. Research in immune modulation aims to prevent graft rejection. These innovations provide patients with safer procedures, faster recovery, and better vision outcomes.
Living with a Transplanted Cornea
Life after a corneal transplant requires careful attention to eye health. Patients should protect their eyes from trauma, UV exposure, and infection. Adherence to prescribed medications and regular check-ups is critical. Temporary adjustments to activities like swimming or contact sports may be necessary. Consistent care ensures long-term success of the transplant. Many patients regain independence and enjoy improved vision. Emotional and social support enhances the adjustment period and overall recovery experience.
Frequently Asked Questions (FAQ)
How long does a corneal transplant last?
Corneal transplants can last 10 to 20 years or longer, depending on the type of procedure and individual health.
Can the transplant be rejected?
Yes. Symptoms include redness, blurred vision, light sensitivity, and discomfort. Early treatment often prevents permanent damage.
Will I need glasses after surgery?
Some patients require glasses or contacts to achieve the best vision, depending on preexisting conditions and healing.
Is the procedure painful?
Anesthesia prevents pain during surgery, and mild soreness may occur during recovery.
When can I resume normal activities?
Light activities resume within weeks, while strenuous activities or swimming may need to wait several months.
Can both eyes be transplanted simultaneously?
Usually, transplants are staged to monitor healing and reduce risks before operating on the second eye.
Takeaway
Corneal transplant surgery offers renewed vision and hope for patients with damaged or diseased corneas. Proper preparation, expert surgical care, and diligent follow-up are essential for success. Advances in surgical techniques, tissue engineering, and postoperative care continue to improve outcomes. Recovery requires patience, protection, and adherence to medical advice. With proper care, patients can regain clarity of vision, improve daily functioning, and enhance overall quality of life. Understanding the procedure, risks, and recovery empowers patients to take control of their eye health. Modern ophthalmology provides life-changing solutions, and a corneal transplant may be the key to seeing the world clearly again.