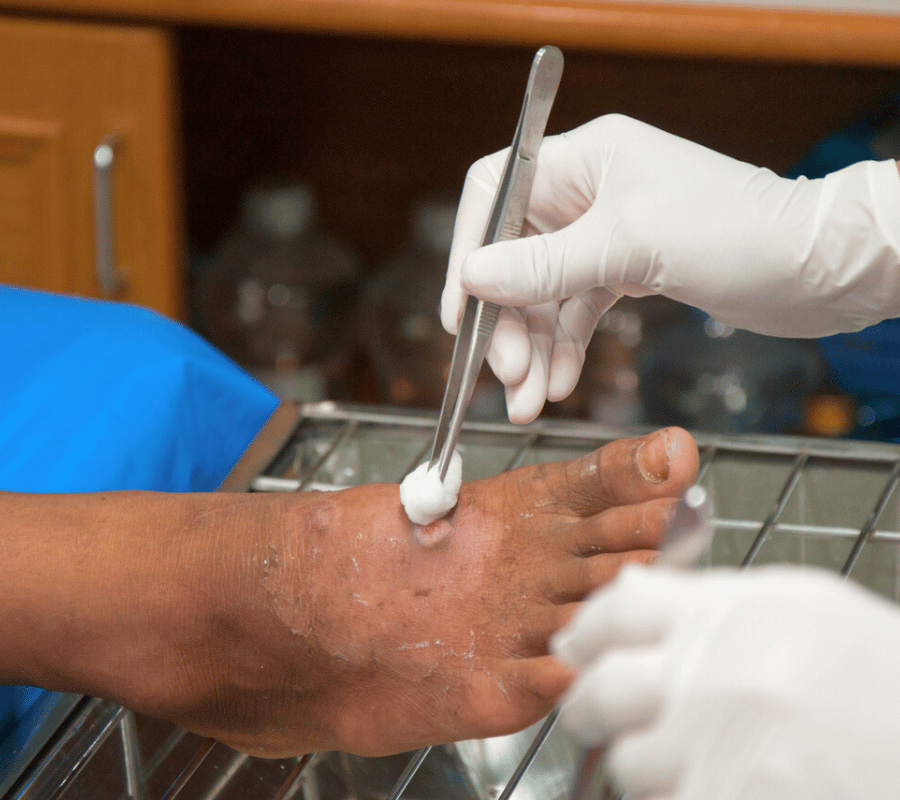
Pressure ulcers, also known as bedsores or pressure sores, can severely impact a patient’s quality of life and increase the risk of serious complications. Proper pressure ulcer management is essential for preventing these wounds, promoting healing, and minimizing pain. Despite the availability of advanced treatment options, many patients and caregivers unintentionally make mistakes that delay recovery. Understanding and avoiding these mistakes is crucial, and partnering with a reputable provider like KALINGAP Wound Care Clinic ensures expert guidance and effective care.
Understanding Pressure Ulcers
Pressure ulcers develop when prolonged pressure restricts blood flow to the skin, causing tissue damage. They are most common in individuals who are bedridden, use wheelchairs, or have limited mobility. Pressure ulcers are classified into stages ranging from Stage 1, which involves superficial redness, to Stage 4, which extends deep into muscle and bone. Recognizing these stages is vital for proper pressure ulcer management, as treatment strategies differ based on severity. Patients who receive timely and accurate care experience faster healing and fewer complications.
Common Mistakes in Pressure Ulcer Management
Even with awareness, certain mistakes frequently occur in pressure ulcer management. Identifying these errors can significantly improve patient outcomes.
Neglecting Regular Skin Assessment
Regular skin inspection is the foundation of effective pressure ulcer management. Failing to monitor high-risk areas like the heels, sacrum, and elbows can result in delayed detection. Early-stage pressure ulcers are easier to treat, making daily skin assessments a critical step in prevention and management.
Inadequate Repositioning and Offloading
Patients who remain in one position for too long are at higher risk of developing pressure ulcers. Proper repositioning and use of pressure-relieving devices such as specialized mattresses or cushions are essential. Without these interventions, wounds may worsen, complicating recovery and extending hospital stays.
Ignoring Nutritional Needs
Nutrition plays a crucial role in tissue repair and pressure ulcer healing. Deficiencies in protein, vitamins, and hydration can slow recovery and increase susceptibility to infection. Comprehensive pressure ulcer management always includes a nutritional plan tailored to the patient’s needs.
Incorrect Wound Dressing Choices
Selecting the wrong type of dressing for a pressure ulcer can hinder healing. Each stage requires specific dressing materials, moisture levels, and infection control measures. Effective pressure ulcer management involves evidence-based dressing protocols and regular reassessment to ensure optimal healing.
Poor Infection Control Practices
Infections are a serious risk in pressure ulcer management. Neglecting hygiene, using non-sterile tools, or delaying medical intervention can escalate minor wounds into severe infections. Consistent infection control and monitoring are essential components of a robust management strategy.
Lack of Multidisciplinary Collaboration
Pressure ulcer management is most effective when healthcare providers, caregivers, and nutritionists work together. Relying solely on one approach or individual can result in incomplete care. A team-based approach ensures comprehensive management and faster recovery.
Practical Tips to Avoid Mistakes
Successful pressure ulcer management depends on prevention, early intervention, and adherence to best practices. Implementing the following strategies can reduce the risk of complications:
- Conduct daily skin assessments, focusing on bony areas
- Reposition immobile patients at least every two hours
- Use pressure-relieving mattresses, cushions, and supports
- Follow evidence-based dressing protocols for each stage of ulcer
- Ensure adequate nutrition and hydration to support healing
- Educate caregivers and staff about early warning signs and proper care techniques
- Maintain strict hygiene and infection control practices
- Collaborate with a multidisciplinary healthcare team
Partnering with a trusted provider like KALINGAP Wound Care Clinic ensures all these strategies are implemented effectively, with guidance from experienced professionals.
Real-Life Examples
Consider a patient who developed a Stage 2 pressure ulcer on the sacral area. Initial care involved infrequent repositioning and improper dressing. The wound worsened over a week, causing severe pain and risk of infection. After engaging KALINGAP Wound Care Clinic, the patient received a tailored care plan including proper dressing selection, daily assessments, nutritional support, and frequent repositioning. Within two weeks, the wound began healing, demonstrating how avoiding common mistakes accelerates recovery.
Tools and Resources for Effective Pressure Ulcer Management
Utilizing modern tools can significantly improve pressure ulcer management outcomes. Pressure-relieving devices, wound assessment charts, and mobile apps for monitoring high-risk patients enhance care quality. Following professional guidelines from organizations like NPUAP and EPUAP ensures treatments are evidence-based. KALINGAP Wound Care Clinic provides access to these tools and guidance on their proper use, making them a reliable partner for both patients and caregivers.
Takeaway
Avoiding common mistakes in pressure ulcer management is essential for preventing complications and promoting faster healing. Neglecting assessments, improper repositioning, poor nutrition, incorrect dressing choices, and lack of collaboration can all delay recovery. Implementing best practices, using the right tools, and seeking expert guidance make all the difference. KALINGAP Wound Care Clinic stands out as a trusted provider for effective pressure ulcer management, offering comprehensive solutions, expert care, and personalized plans to ensure optimal patient outcomes. Prioritizing proper care today can prevent serious complications tomorrow and significantly improve quality of life for those at risk.
FAQs About Pressure Ulcer Management
Q1: What is the best way to prevent pressure ulcers?
Regular repositioning, daily skin assessments, proper nutrition, and the use of pressure-relieving devices are key preventive measures. Professional guidance from KALINGAP Wound Care Clinic enhances these efforts.
Q2: How often should wound dressings be changed?
Dressing changes depend on ulcer stage, exudate level, and dressing type. Following evidence-based protocols and consulting experts at KALINGAP Wound Care Clinic ensures proper care.
Q3: Can pressure ulcers heal completely?
Yes, early detection and proper pressure ulcer management can result in complete healing. Advanced stages may require longer recovery, but expert care significantly improves outcomes.
Q4: Who should be involved in pressure ulcer management?
A multidisciplinary team including nurses, physicians, nutritionists, and caregivers is ideal. KALINGAP Wound Care Clinic coordinates such collaborative care for optimal results.
Q5: Are pressure ulcers always painful?
Pain levels vary depending on ulcer stage and location. Early-stage ulcers may be uncomfortable rather than painful, while advanced stages can cause significant pain.